Results-Driven Medical Billing Solutions
< 30
Days in AR
10-15%
Revenue Increase
97%
First Pass Ratio
96%
Collection Ratios
98%
Clean Claims Rate
Medical Billing Services
Tailored for Your Practice
We understand your unique demands! At MediBillMD, we provide comprehensive billing services for your needs. Our team of experts streamline the billing process by using the latest technology. From small clinics to large hospitals, our tailored solutions cater to all types of practices. We transform your business by offering 100% HIPAA-compliant billing solutions that lead to timely reimbursements. Our medical billing services include:
We minimize your paperwork and financial stress! At MediBillMD, we make sure you get paid for your time and services. Our physician billing services guarantee rightful payments via timely submissions.
We reduce your administrative burdens! At MediBillMD, we know how to tackle different payer policies and requirements. Our team of specialists provides accurate hospital billing solutions, adhering to the ever-changing regulations.
We enhance practice performance! At MediBillMD, we conduct in-depth billing audits to improve your claim submission efficiency. Our audit team analyzes every aspect of your revenue cycle to identify missed opportunities.
We provide unique, affordable, and high-quality billing solutions! At MediBillMD, we customize our billing solutions to your needs. Our experts bring clarity and profitability to your small practice by strengthening your revenue stream.
We optimize your revenue! At MediBillMD, we enhance your billing accuracy through comprehensive CPT coding and reimbursement analysis. Our experts offer precise coding for all services and insightful analysis to identify trends and discrepancies.
We help you avoid penalties due to negligence and malpractice! At MediBillMD, our certified experts meticulously verify your physicians’ educational and professional background, helping you maintain your reputation and a steady cash flow.
We help you minimize coding errors! At MediBillMD, we handle all the tedious tasks, including the accurate recording of service charges. Our medical billing specialists carefully collect all the relevant data to prevent miscommunication.
We bring clarity to your financial status! At MediBillMD, our payment posting service streamlines your payment recording process, providing a clear picture of your revenue cycle so you can identify and resolve major issues.
We address your revenue issues! At MediBillMD, we offer end-to-end RCM solutions to improve the speed and accuracy of your payments. Our team identifies revenue cycle trends so you can enjoy a steady cash flow.
We ensure full reimbursements! At MediBillMD, we retrieve your outstanding accounts receivables. Our special A/R follow-up team tracks the progress of your claims and ensures quick payments of your outstanding amount.
We recover your lost revenue! At MediBillMD, we employ a strong denial management strategy to recover your financial losses. Our specialists review and identify the issues in your rejected claim and correct them for resubmission.
We decrease rejection through accurate verification! At MediBillMD, we fast-track patient eligibility and benefits verification to ensure that every service you render is covered under the patient’s insurance plan. Pre-certifications are obtained when needed.
Why Outsource Medical Billing Services to MediBillMD?

Maintaining an in-house billing department requires hiring and training staff, as well as purchasing software, resulting in a spike in overhead expenses. Start saving by outsourcing medical billing services to MediBillMD for the most affordable rates.
Experienced medical billing specialists at MediBillMD are well-versed in complex coding, billing laws, and payer requirements. Outsourcing medical billing services to experts ensures accurate claim submissions & fewer claim denials.
MediBillMD’s AAPC-certified coders and expert billers optimize your revenue cycle with faster processing and clean claim submissions, resulting in speedy reimbursements and improved cash flow for your healthcare practice.
At MediBillMD, we leverage cutting-edge hardware and software to ensure billing accuracy during electronic claim submissions and use robotic process automation (RPA) for improved efficiency in back-end functions like charge entry.
In accordance with the HIPAA security rule, we prioritize protecting our clients’ and their patients’ confidential information against data breaches. Our systems are password-protected, and all files are end-to-end encrypted.
Medical billing specialists at MediBillMD are aware of changes in healthcare rules and regulations and modify their procedures on an ongoing basis to ensure strict compliance with the revised guidelines, preventing lawsuits.
In-house vs Outsourced Medical Billing Services
Choose better to grow better! The choice between in-house and outsourced medical billing services boils down to a few determining factors like cost, accuracy, efficiency, and collection rate. Understand the impact of in-house vs outsourced medical billing on the financial health of your practice to make an informed decision.
| Outsourced Medical Billing | In-house Medical Billing | |
|---|---|---|
| Cost | The going rate for outsourced medical billing services is between 4% and 10% of net monthly collections. Some, like MediBillMD, charge 2-5%. | The cost of in-house medical billing can range from 7-10% of total monthly collections, including salaries, benefits, and overhead expenses. |
| Clean Claim Rate | The findings of a Medical Group Management Association (MGMA) study revealed that outsourcing medical billing services can increase the clean claims rate to 96.5%. | The same study by the Medical Group Management Association (MGMA) found that the clean claim rate for in-house billing is less, at 94.5% |
| Reimbursements | According to the Journal of Medical Practice Management, outsourcing medical billing services can result in an 80% first submission payment or reimbursement rate. | In the same research, published in the Journal of Medical Practice Management, in-house billing can achieve a 68% first submission payment rate. |
| Billing Accuracy | Outsourcing medical billing services can improve billing and coding accuracy by up to 99%. A team of trained and certified specialists works on your account. | The accuracy rate for in-house medical billing is around 70%. Letting your own staff handle medical billing can lead to errors and coding confusion. |
| Turnaround Time | Medical billing service providers have dedicated teams and can process claims within 24-72 hours, ensuring timely filings and speedy reimbursements. | Claim processing and filing can drag on for weeks when a practice’s preoccupied and overworked in-house staff are assigned the task. |
| Compliance | Third-party medical billing service providers promise 100% regulatory compliance and ensure it to maintain their accreditations, certifications, and memberships | Although regulatory compliance is a must during in-house medical billing, increased workload may lead to oversights, resulting in legal actions. |
Maximize Savings by Outsourcing
Medical Billing
At MediBillMD, we offer comprehensive healthcare billing services at unbeatable prices. We eliminate all the overhead expenses and provide incredible annual savings by charging only for the services offered. Choose MediBillMD and improve your cash flow today.
Calculate Outsourcing Cost
Based on your annual collections, we’ll estimate your in-house billing expenses and reveal your potential savings from outsourcing medical billing services to MediBillMD.
Our Medical Billing Process
We take a systematic approach to file your claim. Our medical billing process is designed to ensure full reimbursements on the first attempt. We work hand in hand with the healthcare providers to file accurate medical claims.
-
1. Requirement Analysis
We begin by determining your practice’s needs, goals, and billing process.
-
2. Patient Registration & Verification
Next, we collect all the relevant information about the patient and verify his insurance coverage.
-
3. Coding
Our certified coders then assign appropriate CPT (Current Procedural Terminology) codes to medical services and procedures.
-
4. Claim Submission
The next step is to submit the medical claim to the appropriate insurance company.
-
5. Payment Posting
Once the claim is processed and the outstanding amount is collected, we record the payments received from the payers and the patients in the system.
-
6. Follow Up
Lastly, we deposit the money to the healthcare providers and submit accurate reports.
Get answers to your questions! At MediBillMD, we offer 24/7 dedicated customer support with all our services. Our staff has the knowledge and expertise to address medical billing and related issues across all specialties.
Whether you are running an individual practice in California or providing services in a healthcare facility in New York, medical billing services are required to get your rightful reimbursements for patient encounters and performed procedures. Trying to handle the clinical and financial aspects can lead to physician burnout, but not if you partner with MediBillMD! We offer tailored healthcare billing services across all 50 states of the US.
Medical Billing Company Trusted by 200+ Practices
Our results speak for themselves! Healthcare providers nationwide outsource medical billing services to MediBillMD, a top-rated medical billing company trusted by 200+ practices across multiple healthcare specialties.
Medical Billing Industry News & Insights
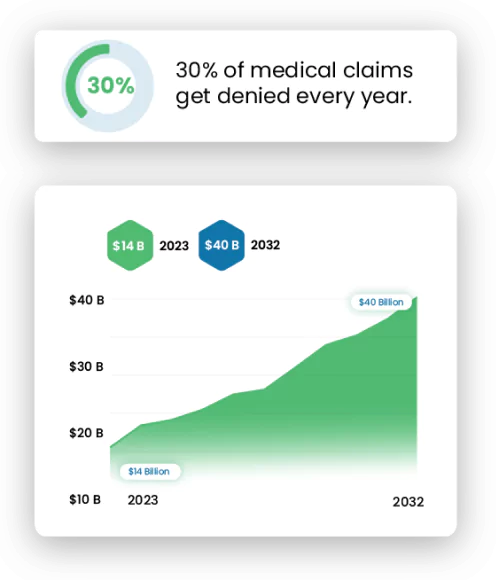
Typically, 30% of medical claims get denied every year. Outsourced medical billing services can reduce them to around 5 to 10%. The best part is that they only charge 2 to 5% of the total net collection.
Medical Billing is an ever-growing industry. Its outsourcing market size was around $14.1 billion in 2023. However, it is expected to increase by 95.9% in the next decade, reaching $40.1 billion by 2032, according to DataHorizzon Research. The following stats provided by Zippia offer valuable information about this industry’s size and structure:
- Medical billing companies function regionally in the US.
- They have an average of 50 employees.
- Medical billing is generally an inclusive industry, employing people from diverse backgrounds and maintaining a balanced gender ratio.
- Around 81% of the employees in this industry are women.
- Hispanics or Latinos make up the most common minority.
Get a Dedicated Billing Specialist For Your Practice
Optimize your revenue cycle to survive in this industry! Choose a dedicated billing specialist like MediBillMD and overcome all the hurdles, including complicated insurance policies, contractual obligations, and changing regulations.
FAQs
You should outsource your healthcare billing process to MediBillMD for the following reasons:
- To improve your cash flow
- To increase your revenue
- To avoid financial losses
- To reduce your claim denials
- To receive quick reimbursements
You can outsource healthcare billing by contacting a reliable provider. This third party will handle all your billing tasks, from collecting relevant information and coding to medical claim submissions at reasonable rates.
You can improve your billing process by outsourcing it to a reliable medical billing company like MediBillMD.
Data breaches are a serious concern in the healthcare sector. Therefore, HIPAA has set some standards to protect your patients’ privacy. Your billing process should comply with HIPAA regulations to avoid costly penalties.
Outsourcing healthcare billing services can improve your profitability by:
- Reducing overhead costs
- Improving your cash flow
- Recovering your lost revenue
- Increasing customer satisfaction