Did you know that on average, it costs $200 to get each provider credentialed in hospitals or practices? Besides, you must re-credential every two to three years to continue providing care to the members of the specific insurance carrier.
Despite how frustrating, expensive, and time-consuming it sounds, credentialing is one of the most important considerations in medical practice management today.
But this blog is not about debating its value. It is about breaking down everything you need to know about the two types of credentialing processes, i.e., solo practitioner credentialing and group practice credentialing. Understanding the two approaches will help you choose the one that best suits you. So, continue reading!
Group Practice Credentialing
Group credentialing is a dual-layered process that synchronizes the business entity with its individual clinicians. Simply put, it applies the hub-and-spoke model, where the entity (group practice) acts as the central hub.
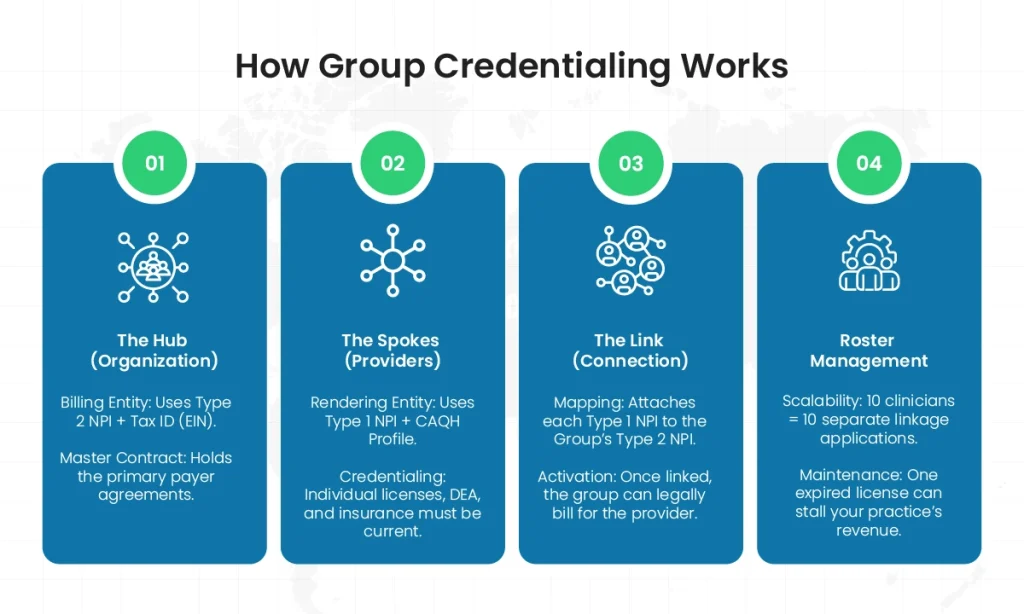
But, how does it work?
- The process of group practice credentialing is initiated by first establishing the group’s identity. That is, you must link a Type 2 NPI to a tax ID (EIN). This sets the stage for your organizational umbrella that holds all your primary contracts with various insurance carriers, such as Medicare, Medicaid, and other private payers.
- Next comes individual synchronization. That is, each healthcare provider, whether it be a physician, nurse practitioner, or physician assistant, must maintain an active Type 1 NPI. That’s not all! They should also have an updated and attested CAQH profile.
- Once the group practice contract is active, the linking phase begins. That is, you must submit each individual healthcare provider’s documentation to the payer to link them to the group’s tax ID.
- Note that roster management is an important part of group practice credentialing. For example, if a group has 10 clinicians, you must submit 10 separate sub-applications. This process relies on a unified roaster. That is, if one provider’s CAQH profile expires, it can delay enrollment and reimbursement for the entire group.
Benefits of Group Practice Credentialing
Discussed below are some of the benefits of group practice credentialing:
Offers Scalability
With group practice credentialing, adding new healthcare providers to your existing group contract is much faster and easier than initiating a new solo application.
Enhances Negotiating Power
How does the size of your practice impact the reimbursement rate? When you are a large practice, you have the leverage to negotiate higher reimbursement rates with private payers.
Enables Centralized Billing
When a group practice is in-network, insurance carriers issue payments to the practice’s tax ID. This not only simplifies the financial reconciliation but also makes revenue tracking efficient for the practice.
Secures Better Returns On Credentialing Investments
What happens when a provider leaves a group practice? Since the credentialing contract belongs to the group, the practice retains the right to bill for that spot. The outcome? You do not lose the money and time you spent on credentialing, ultimately leading to a better return on your investment.
Disadvantages of Group Practice Credentialing
The following are the key challenges associated with group practice credentialing:
Higher Complexity
For group practices, roster management is integral. That is, if a single healthcare provider fails to re-attest their CAQH profile or their license expires, the entire practice takes the blow. These consequences include delayed payment and audit risks.
Shared Liability
When you are credentialed as a group with a payer, all healthcare providers practicing under you share the same reputation. Thus, if any member makes administrative errors, it can affect the group’s overall standing with the payer.
Linking Delays
Yes, adding new healthcare practitioners is easier, but the initial setup of a group contract can take anywhere from 120 to 150 days.
Solo Practitioner Credentialing
Unlike group practice credentialing, solo practitioner credentialing follows a linear, individual-centric approach. It is best for healthcare providers who act as both the clinical lead and business owner.
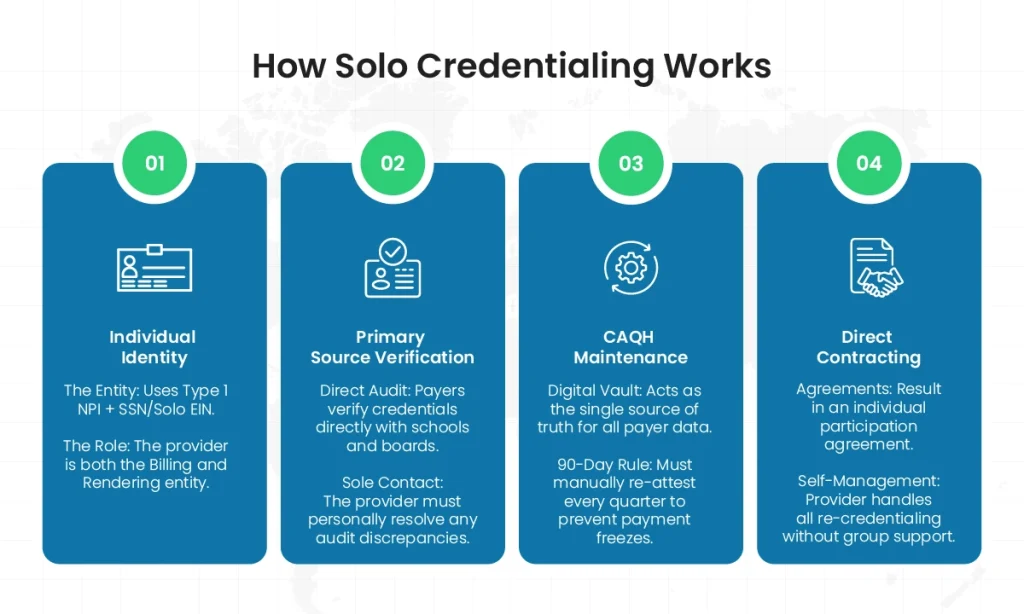
So, how does it work?
- Let’s first understand that the solo practice typically operates under a Type 1 NPI. This means you may have a solo-business EIN, but when you apply as an individual healthcare provider, your relationship with the insurance carrier is tied directly to your professional credentials and standing.
- In the solo practitioner credentialing process, you are the sole point of contact for resolving any discrepancies found during the primary source verification.
- Note that your CAQH profile works as the digital vault. That is, your credentialing success depends on how proactively you re-attest this data every 90 days to prevent silent de-credentialing and automatic claim denials.
- Upon completion of the solo credentialing process, you will enter into an individual participation agreement. This means you are personally responsible for all re-credentialing cycles and contract maintenance without a group administrator’s support.
Benefits of Solo Practitioner Credentialing
Let’s review some of the benefits of solo practitioner credentialing:
Guaranteed Profitability
The best thing when you get credentialed as a solo practitioner with an insurance carrier is that your credentials stay with you. That is, in case you ever transfer to a different office or move to another state, you do not have to reapply.
Simply update your demographic details on your CAQH profile and payer portal, and you are good to bill the specific payer.
Full Control of CAQH Profile
When you apply for credentialing as an individual provider, you become the owner. That is, you have direct oversight of the expiration dates of licenses, deadlines for re-attestation of the CAQH profile, and other payer-related requirements.
The outcome? A seamless credentialing workflow without relying on a group administrator.
Faster Initial Setup
The initial credentialing application is more straightforward for individual providers. Besides, the entire process may take anywhere from 90 to 120 days.
Better Personal Branding
What happens when you get credentialed with payers as a solo provider? Insurance carriers start recognizing you directly. This helps you build your reputation and niche specialty visibility across different payers.
Disadvantages of Solo Practitioner Credentialing
Discussed below are the main challenges you may encounter while getting credentialed as a solo practitioner:
Increased Administrative Burden
As we discussed, when you apply for credentialing as an individual provider, you become the owner and are in full control of your application.
This may sound appealing, but it has its disadvantages. For starters, it increases your administrative burden.
Simply put, you are responsible for every re-credentialing cycle, primary source verification, and document update.
Low Negotiation Power
When it comes to contract negotiations for reimbursement rates, individual providers have the least say. That is, you may have to accept whatever the insurance carriers offer you.
Revenue Gap
Now that you have been focusing on solo practitioner credentialing, what happens when you decide to expand and hire a second provider?
Note that they cannot start seeing patients and billing payers based on your solo credentials. Hence, you will have to wait for months for their solo credentialing process to be completed. Only then can you bill for their rendered services.
Group vs Individual Credentialing – Key Differences
The table below offers an at-a-glimpse view of the key differences between individual provider and group practice credentialing:
| Solo Practitioner Credentialing | Group Practice Credentialing | |
|---|---|---|
| Primary User | Individual healthcare provider. | Clinics, LLCs, multi-provider practices. |
| NPI Required | Type 1 only. | Type 1 (for rendering) + Type 2 (for billing). |
| Billing Entity | The individual provider. | The business/organization. |
| How to Add Providers? | Must reapply for each new provider. | Faster linking to group contracts. |
| Contract Type | Individual participation agreement. | Group/organizational agreement |
Let’s understand the key differences in detail:
1. The Identifier Setup
The most technical difference lies in how the payers recognize you in their systems.
- For Solo: The insurance company uses a Type 1 NPI along with your social security number (SSN) or a solo-business EIN. Besides, the payer releases all reimbursements directly to the individual provider.
- For Group: If you want to get credentialed as a group practice, you need a Type 2 NPI and a business tax ID (EIN). Note that the individual clinicians working for you still require their Type 1 NPI as the rendering providers. However, your group NPI will be the entity to whom the payer will send the payment.
2. Portability vs. Practice Retention
Cost is another factor that comes into play while deciding whether you should go for group or solo credentialing:
- For Solo: Let’s say that individual provider credentialing is portable! That is, no matter where you move (to a private clinic, a hospital, or a different state altogether), your in-network status often follows you. You will most likely only require a simple demographic update with the insurance carrier.
- For Group: The credentialing status is tied to the group contract. As a result, if any healthcare provider leaves the group, they may lose their in-network status with certain payers.
3. Scalability and Onboarding
Another distinction is in the process itself:
- For Solo: Every new hire must go through the full 90-120-day application process from scratch. That is, there is no shortcut for adding a second or third provider.
- For Group: Once the group contract is established, linking (adding new providers) becomes easier. Besides, it typically takes only 30-60 days.
4. Negotiation and Reimbursement Rates
Your negotiation power varies significantly depending upon whether you are applying as a solo practitioner or a group practice:
- For Solo: Individual healthcare providers do not have much say in the reimbursement rate. Thus, you are typically offered the standard fee schedule.
- For Group: Multi-specialty and large group practices have better negotiation power. That is, insurance companies are often willing to offer higher reimbursement rates to groups that can provide a wide range of services or a high volume of care in a specific region.
Partner With MediBillMD to Streamline Credentialing
Phew! Too many details to digest. Hopefully, this guide will clear the fog and help you understand which credentialing approach is better for your medical practice.
But keep in mind that regardless of the approach you choose, credentialing is a time-consuming process and demands constant follow-ups. Without a credentialing specialist or a dedicated staff to respond to every payer query, your credentialing request can be further delayed, straining your revenue cycle.
Thus, if you do not want to experience payment delays, feel free to outsource insurance credentialing services to professionals, like MediBillMD.



